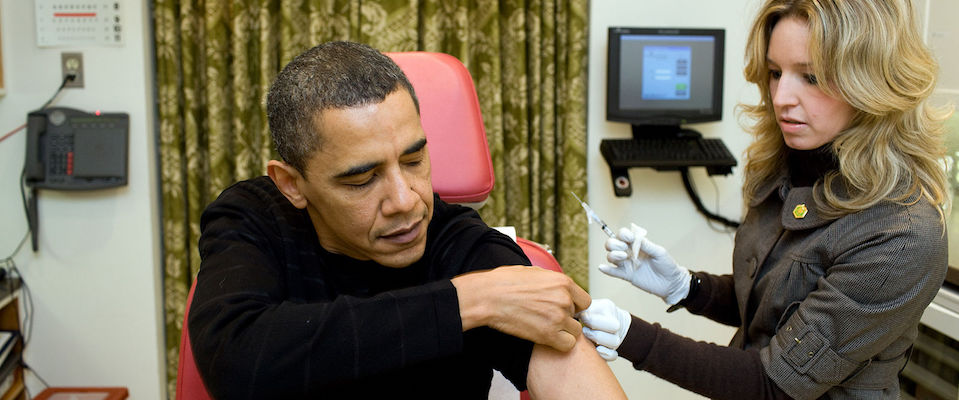
As a UC Berkeley School of Public Health emeritus professor specializing in infectious diseases, John Swartzberg knows viruses as well as other people know their lapdogs. So when he gets concerned about a bug, so should you. And right now he’s pretty concerned about measles. Anyone who has perused a news site or suffered through a CNN broadcast over the past week can guess why: An outbreak of measles that erupted in Disneyland now has spread to at least seven states and resulted in almost 100 cases, with no sign of abating.
Sure, measles isn’t Ebola or Lassa fever, or even a nasty strain of influenza. But it isn’t the viral equivalent of a hangnail, either. Swartzberg cites some supporting evidence:
- Measles is among the most contagious of viral diseases, with the average infected person capable of infecting 12 to 18 unvaccinated people.
- Measles can cause real misery. In the decade before measles vaccination began in the United States, 3 to 4 million citizens were infected annually. Of that number, around 48,000 were hospitalized, about 1,000 developed chronic disability from measles encephalitis, and 400 to 500 died.
- Measles is easily transmitted—and potentially devastating—to children who are too young to receive vaccinations, and to people for whom vaccination is a legitimate risk, such as patients with severe immune deficiencies.
- Measles epidemics are expensive. A 2004 Iowa outbreak involved only three confirmed cases, but their treatment and the investigation required to confirm their contacts cost local and state health departments more than $140,000. The costs involved in addressing a handful of confirmed cases during a 2008 outbreak at two Arizona hospitals hit $800,000.
“The current outbreak can’t be considered momentous in terms of mortality, but it’s still a very large red flag for the U.S. public health system,” says Swartzberg. “It says there are far too many people in our nation who aren’t protected from disease by immunization. We don’t have that herd immunity that widespread vaccination once provided.”
Indeed, until the recent rash of outbreaks, measles was eliminated from the United States. That’s not the same thing as eradicated, Swartzberg observes. Eradication means zero cases, period. In the medical context, elimination is the absence of “autochthonous” cases: Infections that were not imported, but arose from native sources. The Happy Kingdom’s outbreak, it’s believed, originated from foreign tourists.

Still, the chances of an outbreak would have been almost nil if everyone at Disneyland had been up-to-snuff on their inoculations. That’s because the measles vaccine is 95 percent effective in preventing infection. Swartzberg provides one qualifier: For people who’ve gone decades following their initial vaccination, an extra jab doesn’t hurt (in the public health sense, at least).
“A second injection takes immunity from 95 percent to 97 to 99 percent,” he says. “For most infectious diseases, 95 percent is fine. Even for measles, the target for herd immunity is 95 percent. But given that measles is one of the most contagious diseases around, that extra few percent can make a huge difference when there’s an outbreak.”
And of course, we’re not at the 95 percent vaccination rate—for measles or any other infectious disease. According to the state Department of Public Health, about 90.4 percent of California’s kids were up-to-date on their vaccinations in 2014. That’s well under the figure needed for herd immunity.
Which brings up the 800-pound public health gorilla in the room: The anti-vaccination movement. Swartzberg has had it up to here with anti-vaxxers, and he’s taking off the (surgical) gloves.
“A small but very vocal minority is perpetuating this myth (the danger from vaccines), and we have to stop accommodating them,” Swartzberg says. “As with climate change, there is no legitimate debate. Both climate change and the efficacy and safety of vaccinations are as real as the sun rising.”
Swartzberg acknowledges he is particularly exasperated with media coverage of vaccination issues.
“Physicians need to do a better job debunking this disinformation, and politicians also must be held to account. Though anti-vaccination activists are few in number, they are extremely vocal.”
“On a recent story broadcast on KQED, the director of public health for Marin County and a chiropractor who opposed vaccination were given equal time, as though their credentials were equivalent,” he says. “I was astounded.”
But it’s not just newshounds seeking “balance” who are to blame, Swartzberg emphasizes.
“Physicians need to do a better job debunking this disinformation, and politicians also must be held to account. Though anti-vaccination activists are few in number they are extremely vocal, and they carry disproportionate weight with politicians.”
Swartzberg observes he was disappointed with Gov. Jerry Brown’s response to AB 2109, a 2012 bill that required anyone seeking a “philosophical exemption” from school vaccination mandates to obtain a signed attestation from a physician that vaccination counseling had been provided. Brown signed the bill, but added the addendum:
“…Additionally, I will direct the department to allow for a separate religious exemption on the form. In this way, people whose religious beliefs preclude vaccinations will not be required to seek a health care practitioner’s signature…”
And that, of course, nullified any significant impact the law may have had.
Vaccination proponents do appear to be making incremental headway. That 90.4 percent vaccination rate cited by the California Department of Public Health represents a 0.2 percent increase from the previous year.
“If there’s a silver lining on the current measles outbreak, it’s that there should be an uptick in vaccinations,” Swartzberg says. “Unfortunately, it may only be transient. The irony in this entire process is that success is determined by things not happening. If a surgeon performs a successful procedure, the patient is very aware of it. But no one has ever thanked me for not getting pneumococcal pneumonia because I gave them an anti-pneumonia vaccine. The benefits of vaccinations are profound, but they often are not apparent to the public.”